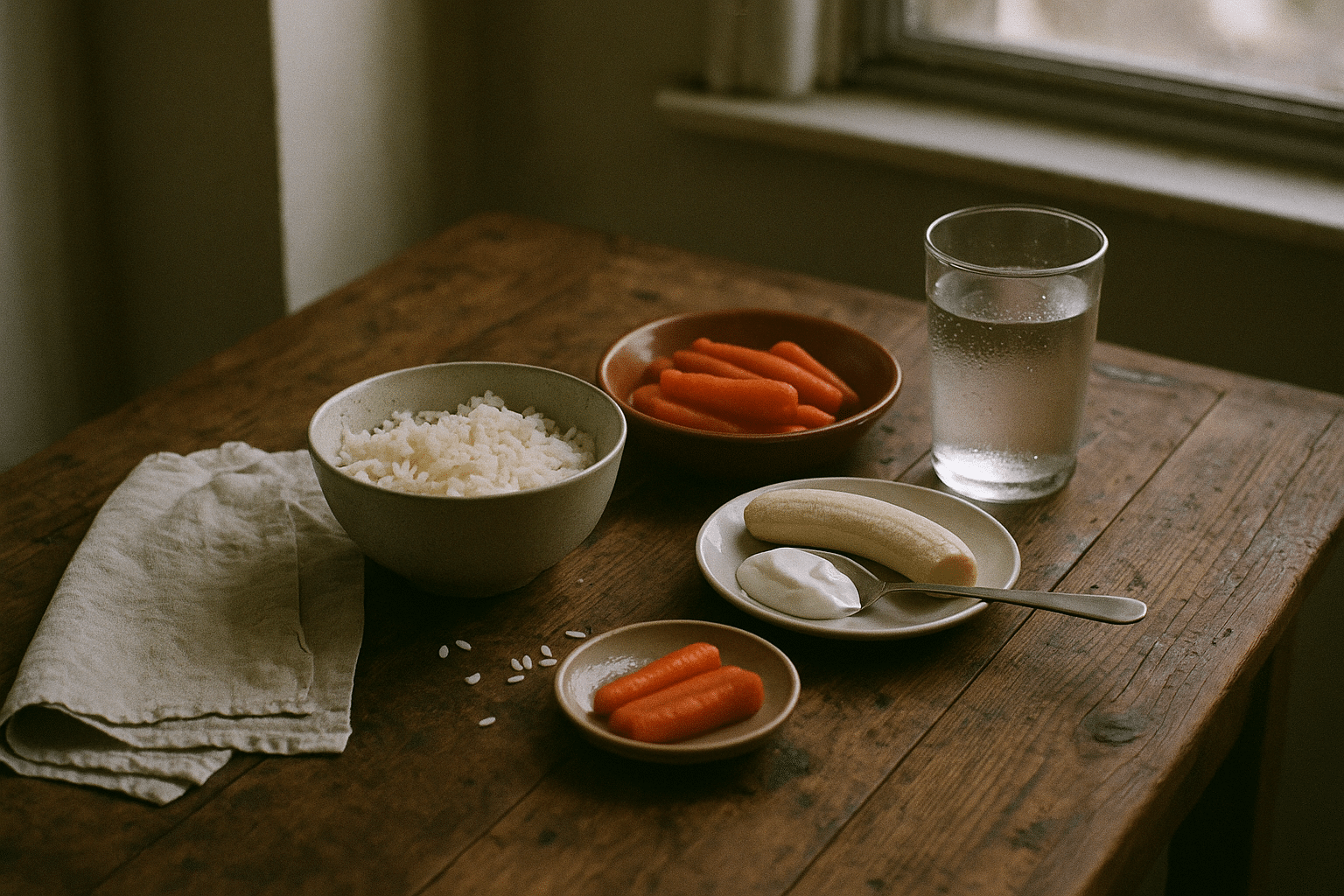
5 Foods to Be Careful With If You Have Colitis
Outline:
– Food choices and symptom patterns: why certain items can stir up trouble, plus practical swaps
– Core ulcerative colitis treatment paths: medicines, monitoring, and cost-aware decision-making
– Personalizing your plan: tracking triggers, telehealth coordination, and smart budgeting for labs
– Working the system: networks, billing details, and when to escalate care
– Meal planning that respects symptoms and your wallet, with insurance-supported nutrition help
Food Triggers to Approach Carefully (And Smarter Swaps)
Ulcerative colitis affects the lining of the colon, so anything that increases irritation or motility can amplify discomfort during active disease. Not everyone reacts the same way, yet patterns do emerge. Rather than rigid “never eat” lists, it helps to recognize common culprits and test them methodically. Below are five food categories many people with colitis approach cautiously, especially during flares, alongside ideas that feel gentler on the gut.
– Spicy chilies and hot sauces: Capsaicin can speed transit and heighten burning sensations. If you love heat, try a mild sprinkle of smoked paprika or roasted red pepper purée for depth without the same kick.
– Tough, insoluble-fiber roughage: Raw kale, broccoli stems, cabbage salads, and popcorn can be abrasive during flares. Swap in peeled, cooked carrots, squash, ripe bananas, and well-cooked oatmeal to lower mechanical irritation while keeping nutrients.
– Dairy for those with lactose sensitivity: Inflammation can unmask lactose intolerance. Consider lactose-free milk or small portions of hard cheeses or yogurt with live cultures, introduced when stable.
– Alcohol and excess caffeine: Both may stimulate the bowel and increase urgency. Opt for decaf tea, diluted smoothies, or electrolyte water during recovery days.
– Sugar alcohols and ultra-processed, high-fat items: Sorbitol, mannitol, and very greasy meals can trigger gas and diarrhea. Choose simple carb sources like white rice or toast and lean proteins such as poached fish or eggs.
Evidence from nutrition research suggests reducing poorly absorbed fermentable carbs (often called “FODMAPs”) can lessen functional gut symptoms in some individuals, though strategies should be individualized for inflammatory bowel disease. The practical path is a structured experiment: change one variable at a time, keep a calm routine for several days, and note stool frequency, urgency, and abdominal pain. A small shift—like steaming vegetables or peeling fruit—can improve tolerance without sacrificing variety.
Most important: food is only one piece of management. Medications control inflammation; meals support comfort and energy. Ulcerative colitis nutrition counseling with a registered dietitian can support flare management while you compare health insurance coverage options. That way, your plate, your plan, and your budget move in the same direction.
Ulcerative Colitis Treatment Paths: Medicines, Monitoring, and Goals
Therapy for ulcerative colitis aims to calm inflammation, achieve remission (few or no symptoms, reduced bleeding), and maintain mucosal healing to prevent complications. Care often follows a step-up approach that considers disease severity, extent, and prior response. Classes commonly used include:
– Aminosalicylates for mild to moderate disease, often as first-line agents.
– Short courses of corticosteroids for flares; they are not a maintenance solution due to long-term risks.
– Immunomodulators that can help maintain remission in selected cases.
– Biologics and small-molecule therapies that target immune pathways, appropriate for moderate to severe activity or steroid dependence.
Choosing between options involves balancing symptom control, safety profile, convenience (oral vs injection vs infusion), and time to response. Clinicians increasingly use a “treat-to-target” strategy: set clear milestones (fewer bowel movements, no visible blood, lab markers improving), check progress at defined intervals, and adjust promptly. Monitoring might include bloodwork (complete blood count, inflammatory markers), stool calprotectin to gauge intestinal inflammation, and periodic endoscopy for objective healing and cancer surveillance over the long term.
Cost and access matter—both can shape adherence. Review prescription drug plan formularies for ulcerative colitis meds, as biologic therapy costs and copays can vary widely by insurer. Ask about prior authorizations, step therapy rules, and infusion center billing. Some plans differentiate between specialty pharmacy shipments and clinic-administered drugs, which can influence out-of-pocket charges. If affordability becomes a barrier, tell your care team early; there may be alternative dosing schedules, therapeutic equivalents, or financial navigation resources that keep treatment on track.
Finally, remember that remission is the north star. Medicines reduce the inflammatory fire; nutrition and stress management can help you stay steady. Regular follow-up—especially after a flare or medication change—allows small course corrections before problems become big ones.
Personalizing Your Plan: Tracking, Telehealth, and Lab Budgeting
Symptoms rarely move in a straight line, which is why a simple tracking system can be transformative. Note the date, bowel movement frequency, presence of blood or mucus, urgency, abdominal pain, and energy level. Add what you ate and any new medications or supplements. After two to three weeks, patterns often surface—perhaps raw salads bother you on days after poor sleep, or carbonated drinks coincide with cramping.
To make this sustainable, use tools you already like: a notes app, a calendar template, or a printed log on the fridge. Track trigger foods with your gastroenterologist via telehealth visits, and budget for lab tests using HSA or deductible planning tools. With scheduled check-ins, your clinician can spot early warning signs (like creeping calprotectin) and adjust therapy before a full flare. When symptoms stabilize, the same data supports careful reintroduction of foods for a more varied diet.
Consider these pragmatic tips:
– Establish a baseline week: eat a gentle, predictable menu to identify your “quiet gut” pattern.
– Change one thing at a time: test a single food or spice for three to four days before adding another.
– Coordinate labs with benefit resets: if your deductible is nearly met, clustering necessary tests may reduce cumulative costs.
– Plan for travel or busy weeks: pre-pack tolerated snacks (rice cakes, bananas, hard-boiled eggs) and keep hydration front and center.
Lab markers guide decisions but don’t replace your lived experience. Communicate how you feel, not just numbers. If you track consistently—even imperfectly—you’ll give your care team a clear map that makes appointments faster, calmer, and more effective. In the long run, this habit trims surprise expenses and prevents avoidable detours.
Working the System: Networks, Billing Details, and When to Escalate Care
Healthcare logistics can be as stressful as symptoms, yet a few administrative moves can protect both your health and your wallet. First, verify that your gastroenterologist and infusion or endoscopy sites are in-network. If colitis symptoms worsen after certain foods, consider an in-network GI clinic and review medical billing, CPT codes, and coverage limits. Ask whether referrals or prior authorizations are needed for procedures. For endoscopy, clarify what’s billed separately: facility fee, professional fee, anesthesia, pathology. Understanding these components keeps the final statement from feeling mysterious.
Bring targeted questions to scheduling calls:
– Which services are billed as preventive versus diagnostic, and how does that affect copays?
– Are telehealth follow-ups covered at the same rate as in-person visits?
– If a procedure changes mid-visit (biopsy added), how does coding shift?
– Do you have an estimate of out-of-pocket costs and payment plan options?
Know the red flags that warrant urgent care: fever with severe abdominal pain, persistent bleeding leading to lightheadedness, dehydration from frequent diarrhea, or rapidly worsening symptoms despite medication. For many people, a same- or next-day clinic visit can avert an emergency department trip—but don’t delay if you feel unstable. Keep a simple folder (paper or digital) with your latest med list, allergies, and recent lab results so any clinician can act quickly.
Finally, track how changes in insurance (open enrollment, job transitions) alter coverage rules. Formularies, network rosters, and coinsurance percentages evolve year to year. A short review each season pays dividends when you need timely care, predictable costs, and fewer surprise bills.
Meal Planning That Respects Symptoms and Your Wallet
Building a week of meals that feels soothing, satisfying, and affordable starts with gentle building blocks. During a flare or sensitive stretch, people often tolerate low-fiber, low-fat, and mildly seasoned dishes. Think simple proteins (poached chicken, baked white fish, soft scrambled eggs), refined grains (white rice, sourdough toast, small pasta portions), and tender produce (peeled zucchini, mashed potatoes, ripe bananas). As symptoms settle, expand slowly: reintroduce cooked spinach, canned peaches in juice, or small servings of nut butters, testing tolerance carefully.
Smart shopping and prep ideas:
– Cook once, eat twice: roast chicken for dinner, then shred leftovers into a mild rice soup.
– Choose multipurpose staples: rice, eggs, and carrots can anchor breakfasts, lunches, and sides.
– Stock an “easy day” shelf: clear broth, instant oats, applesauce, and electrolyte packets for times you need low-effort comfort.
– Flavor with low-heat seasonings: herbs, a squeeze of lemon, or a spoon of roasted garlic purée (if tolerated) can lift a plain plate.
Don’t overlook coverage that can underwrite expert guidance. Medicare Advantage and commercial health plans may offer dietitian visits for ulcerative colitis, which could reduce out-of-pocket nutrition costs. When booking, ask whether virtual counseling is available and how many visits are included per year. Keep receipts and explanations of benefits organized; if a claim is denied due to coding, a quick resubmission with the correct diagnosis can change the outcome.
Finally, weave meals into your medical plan. Set reminders to take medicines with food when indicated, and space fiber supplements away from other pills if advised by your clinician. Hydration deserves top billing: small, frequent sips of water or oral rehydration solutions can make a noticeable difference in energy and stool consistency. Your menu doesn’t have to be boring—it just has to be kind while your gut heals.
Conclusion: Confident Steps Toward Calmer Days
Food choices, medicines, and money decisions all intersect in ulcerative colitis care. By identifying likely triggers, following an evidence-guided treatment plan, and using your coverage strategically, you create a steadier routine with fewer surprises. Pair clinical follow-up with practical meal planning, keep communication open with your care team, and let data from your own diary guide the small adjustments that add up to big relief over time.


